Midfoot Arthritis
Summary
Midfoot arthritis is characterized by pain and swelling in the midfoot, aggravated by standing and walking. There is often an associated bony prominence on the top of the foot. Usually the symptoms develop gradually over time, although it can occur following a major midfoot injury, such as a Lisfranc injury. Non-operative treatment consisting of use of a stiff-soled comfort shoe, activity modification, and weight-loss, can be quite effective. If non-operative treatment fails, patients may benefit from surgery to fuse the arthritic midfoot joints.
Midfoot Arthritis Summary Handout
Background
The foot consists of 26 separate bones working together to bear body weight. Where they link together, one finds cartilage that helps smooth their motion as they move past each other. As one might imagine, there is a significant amount of force that crosses these joints during normal daily function, as the foot acts to propel us forward during walking or running. If this cartilage wears out, a condition known as arthritis, force across these joints may generate pain as bone starts to rub against bone. The “midfoot” portion of the foot is analogous to the articulation, or joint formation, between our wrists and hand. Tarsal bones, specifically the cuneiforms and cuboid, articulate with the long, tubular metatarsals that form the forefoot. Most of the joints of the midfoot are held together by strong ligamnets and move relatively little. When arthritis affects the midfoot joints, it is known as midfoot arthritis.
Clinical Presentation of Midfoot Arthritis
Patients with midfoot arthritis experience discomfort in the midfoot. Symptoms are often aggravated by prolonged standing or walking. Pain can also be exacerbated by shoes with stiff uppers that push downwards on the top of the foot. Some patients also report pain with the first few steps in the morning or after prolonged sitting, traditionally referred to as “start-up” pain. Occasionally, there is a history of significant injury to the midfoot, such as a Lisfranc injury. More commonly, midfoot arthritis occurs due to gradual wear and tear from the repetitive loading of walking as some foot shapes tend to concentrate force across certain midfoot joints leading them to become arthritic over time.
Physical Examination of Midfoot Arthritis
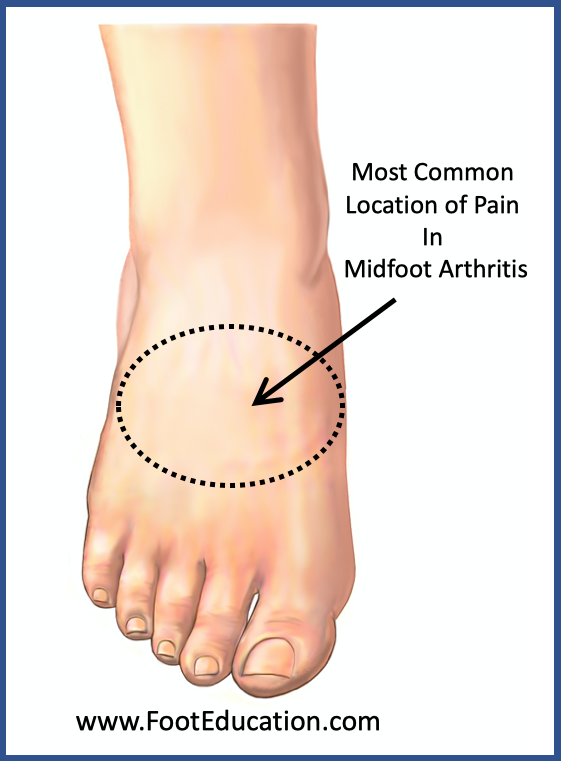
Physical examination may reveal swelling in the midfoot, but more commonly there is often generalized tenderness in the midfoot area (Figure 1), especially over the affected joints. A bony prominence in the midfoot known as an osteophyte is often palpable as a result of the underlying arthritis.
It is important to note, however, not all bony prominences in the midfoot represent arthritis. It is not uncommon for people to have local shoe wear irritation from a normal bony prominence, known as a tarsal boss. This does not necessarily signify significant midfoot arthritis.
Imaging Studies
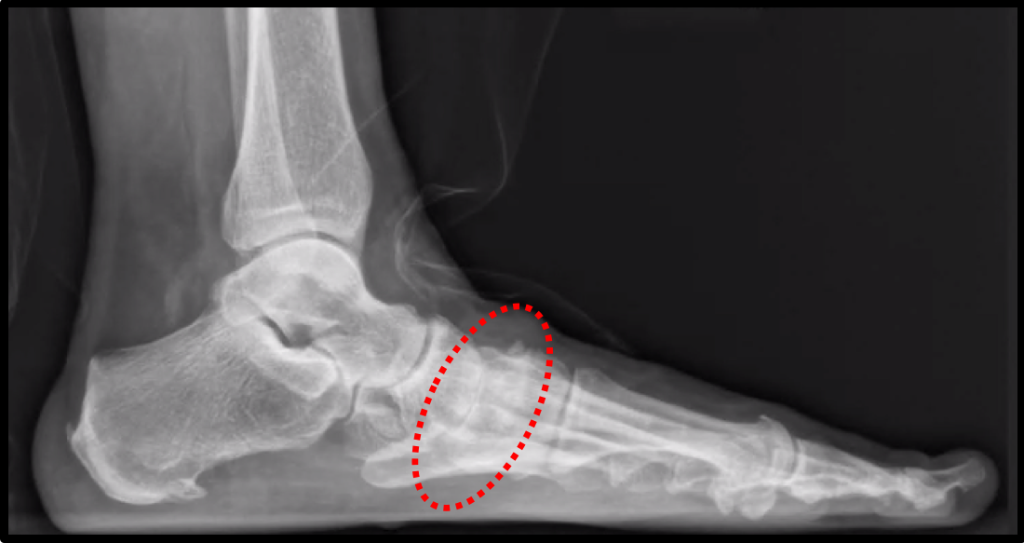
Weight-bearing x-rays generally demonstrate loss of joint space in the affected midfoot joints, which is characteristic of arthritis (Figure 2). The joint between the midfoot and forefoot (tarsometatarsal joint) is most commonly involved, although the other joints may also become arthritic.
Treatment
Non-Operative Treatment of Midfoot Arthritis
Midfoot arthritis can often be managed successfully without surgery. The key components of non-operative treatment are:
- A stiff-soled comfort shoe: By having a stiff sole, the amount of force concentrated in the midfoot will be limited. In a similar manner, a slight rocker contour to the shoe will help disperse the force away from the midfoot and smoothly up the leg.
- Shoes with a softer upper: If the upper portion of the shoe is made out of a mesh-like material rather than a stiff leather, the direct pressure over the arthritis may be lessened and thereby the pain improved.
- Avoid tying shoe-laces too tightly: If shoelaces are kept somewhat loose, less pressure is placed on the arthritic midfoot. Skip-lacing may be helpful if there is a prominence over the midfoot. By skipping one or two holes when lacing a shoe pressure can be taken off a midfoot prominence.
- Activity Modification: Activity modification, such as avoiding rigorous impact activities like running or prolonged walking, may also be helpful in limiting symptoms. Non-weight-bearing exercise (ex. swimming, aquarobics, stationary bike) is encouraged to help keep active and lose weight.
- Weight-loss: Losing excess weight will help to decrease the amount of force going through the arthritic midfoot with each step.
- Calf Stretching (Flexibility improvement of adjacent joints): Unnecessary motion or stress through the midfoot can be decreased by stretching the calf muscle (gastrocsoleus complex and heel cord)
- Anti-inflammatory Medications: Non-Steroidal Anti-Inflammatory medications (NSAIDs) may also be beneficial in improving pain symptoms.
- Off Loading: Decreasing the load through the midfoot by using assistive devices such as a cane, a knee walker, or crutches may be helpful in the short-term if the symptoms have flared up.
- Injections: Periodic corticosteroid injections into the affected midfoot joints may help alleviate pain symptoms, albeit usually only temporarily.
Operative Treatment
Patients may have two problems arising from midfoot arthritis; pain on the dorsum (top) of the foot due to spurs from the arthritic joint (bony prominence), worse in closed shoes or, pain arising from the arthritic midfoot joints.
Symptoms due to a local bony prominence may benefit from removal of bone spurs, though this is uncommonly performed because it does not change the underlying arthritis and the bone spurs generally recur.
In most cases, pain arising from the arthritic joint is the main symptom. Therefore, if an operation is deemed necessary the affected joint usually needs to be fused (midfoot fusion). This entails roughening up the opposing bone surfaces and fixing the bones together with plates, screws, and/or staples in order to get the two bones to fuse together into one larger bone. By eliminating the movement through the arthritic joints, the pain originating from these joints is eradicated. Essentially, it converts a painful stiff joint into a painless stiff joint. However, a midfoot fusion does not preclude pain from other joints and other areas of the foot from continuing to be symptomatic. This type of midfoot fusion surgery requires strong fixation and a period of non-weight bearing (or limited weight bearing) for 6-12 weeks.
Potential Complications
Complications of surgery may include:
- Nonunion (bones do not heal together)
- Delayed union (bones are slow to heal together)
- Infection
- Wound healing problems
- Nerve injury or irritation
- Deep Vein Thrombosis (DVT or Blood clot)
- Pulmonary embolism (PE)
- Removal of hardware
- Adjacent joint arthritis, the nearby joints may develop arthritis over time as a consequence of altered foot biomechanics from arthritis and joint fusion.
In addition, patients may have persistent pain, as the fusion of the midfoot joint will not help pain that originates from other areas of the foot, such as tendons, ligaments, or other joints.
Edited October 30th, 2024
(Previously edited by Daniel Guss, MD, MBA, Peter Stavrou MD, Mark Perry MD and Robert Leland MD)