Subtalar Arthritis
Edited by Michael Castro MD
Summary
Watch Video: Subtalar Arthritis Introduction
Subtalar arthritis is characterized by pain in the hindfoot that is aggravated by standing and walking, particularly on uneven ground. It is likely to be associated with stiffness when attempting to move the foot from side to side. The location of the pain is commonly just below the level of the inside and outside ankle bones (medial and lateral malleoli). The most common cause of subtalar arthritis is a previous injury – usually a calcaneal fracture, or abnormal alignment of the heal bone.
Non-operative treatment involves: 1) limiting the movement and loading through the subtalar joint by wearing comfort shoes, bracing the hindfoot and weight control; 2) activity modification such as decreasing standing and walking, particularly on uneven terrain; and 3) masking the pain by taking NSAIDs, if tolerated, to improve pain control. Surgery is indicated for subtalar arthritis that has failed non-operative treatment. Fusion of the subtalar joint is the most predictable surgical option, as it trades painful motion for relief of pain and improved function.
Clinical Presentation
Patients with subtalar arthritis will complain of pain on one or both sides of the foot, just below the ankle bones (malleoli). This is commonly illustrated by the patient encircling the affected foot with their fingers, just below the level of the bony prominence on either side of the ankle (malleoli). The hollow just in front of the outside ankle bone (the sinus tarsi) is another common location of pain. The sinus tarsi is a space surrounded by the three contact areas between the talus and calcaneus, that comprise the subtalar joint. The subtalar joint is largely responsible for allowing the foot to accommodate uneven terrain by moving the hindfoot from side to side (inversion and eversion). Walking on uneven surfaces places a great deal of stress on the subtalar joint and may be difficult, if not impossible, to accomplish in patients with subtalar arthritis.
Most subtalar arthritis is caused by a previous trauma, usually a calcaneal fracture, although certain fractures involving the talar body may also cause subtalar arthritis. Other causes include rheumatoid arthritis, or the abnormal loading of the subtalar joint associated with malalignment of the heel bone (calcaneus). The load applied to the subtalar joint can be unevenly distributed in cases where the heel bone turns in (varus alignment seen with a high arched foot) or out (valgus alignment associated with a flat foot).
Physical Examination
On examination, patients with subtalar arthritis will usually have noticeable stiffness when testing side-to-side motion. Additionally, this motion may cause pain in the locations described above. There may also be swelling that may bulge above the shoe line.
Imaging Studies
X-rays will reveal a loss of the subtalar joint space that is best seen on a lateral view of the foot, taken with the patient bearing weight (Figure 1).
Figure 1- Subtalar Arthritis
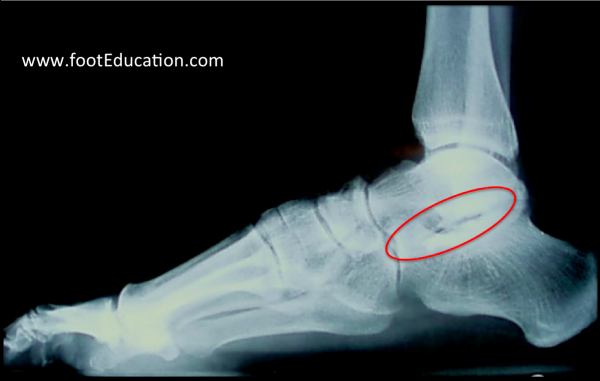
A CT scan or MRI is sometimes indicated to identify the extent of the subtalar arthritis and to determine if there is any other source of pain (ex. ankle arthritis, posterior tibial tendonitis, peroneal tendonitis, etc.)
Occasionally, a diagnostic injection of local anesthetic (ex. lidocaine) will be performed to get some sense of how much pain is originating from the subtalar joint. In some cases, the injection may be given with aid of ultrasound, fluoroscopy (mini x-ray), or CT scan, to ensure that the anesthetic agent is accurately placed. The lidocaine will only last a few hours and when it wears off the pain may actually be worse for a short while. However, if immediately after the injection the patient has significant relief of pain for a few hours, this suggests that most of the symptoms are coming from the area that was injected – in this case the subtalar joint.
Treatment
Non-Operative Treatment
Watch Video: Subtalar Arthritis Non-Operative Treatment
Non-operative treatment focuses on limiting the amount of loading and movement at the subtalar joint, and masking the pain. Non-operative treatment involves some trial and error on the part of the patient to see what strategies are most effective. Non-operative treatments include:
- Activity Modification: Limiting standing and walking, particularly on uneven terrain, will help limit exacerbation of symptoms from subtalar arthritis. Use of an exercise bike or swimming as a form of aerobic exercise instead of walking or running, will likely be beneficial as it allows for a good workout with much less loading through the subtalar joint.
- Weight-Loss: The back part of the foot is subject to forces equivalent to 3-5x body weight during daily activities, so losing even a moderate amount of weight can substantially decrease the forces going through the arthritic joint.
- Comfort Shoes: Use of comfort shoes, including adding a shock absorber in the heal, can help decrease the repetitive loading through the subtalar joint.
- Ankle Bracing: Use of an ankle brace, such as an ankle lacer, or even taping the ankle and hindfoot can be helpful because it serves to limit motion through the arthritic subtalar joint.
- Icing and Elevation after Activity: Elevating the leg and placing a bag of ice around the ankle and hindfoot after activity can help to decrease pain and swelling. Ice should only be applied for 10-15 minutes at a time.
- Anti-inflammatory medication (NSAIDs): If there are no contra-indications, NSAIDs can help decrease a patient’s arthritis symptoms
- Tylenol: Plain Tylenol (acetaminophen) taken 2-3 times a day can help reduce the pain from subtalar arthritis. It may not be as effective as anti-inflammatory medications (NSAIDs), but it works via a different mechanism so it may have an additive effect. It should not be taken by anyone with liver problems
- Glucosamine Sulfate: Although it has not been shown to be beneficial in long-term studies, many people report improved symptom control when they take glucosamine sulfate. It needs to be taken daily for 6-8 weeks for any benefit to be seen.
- Corticosteroid Injections: Pain relief from corticosteroid injections will tend to be temporary.
- Hyaluronic Acid Injections (HA): Injections of HA have shown some success in the knee joint, but the results in the subtalar joint has not been demonstrated.
- Self-Administered strengthening and stretching programs: Exercise to keep the muscles of the foot as strong as possible, and to keep the joint moving through a gentle range of motion, may be helpful.
Printable Summary Handout of Non-Operative Treatment of Foot and Ankle Arthritis
Operative Treatment
Operative treatment is usually reserved for extensive subtalar arthritis that has failed non-operative management. Occasionally patients will be noted to have an isolated area of damage to the subtalar joint, or will have a loose body which can be addressed by cleaning out (debriding) the subtalar joint, either arthroscopically or more commonly by opening the joint. However, in most instances, patients with subtalar arthritis have lost significant cartilage and need to have the subtalar joint fused (Figure 2).
Figure 2: Subtalar Fusion
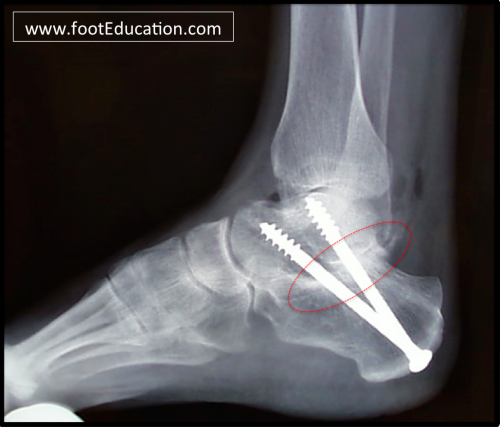
A subtalar fusion is not to be confused with a subtalar arthroresis (placing a plug in the subtalar joint), which is not appropriate for treating subtalar arthritis.
- Subtalar Fusion (Arthrodesis): Fusing the subtalar joint is an effective treatment option for patients with significant subtalar arthritis that has failed non-operative management. When considering subtalar fusion, realize you are trading painful motion for pain relief. Even though the foot will lose side-to-side motion, often patients are able to be much more active because they have substantially less pain.
- A subtalar fusion is performed by cleaning out the remnants of cartilage from the joint, and putting screws and bone grafts across the joint. The goal is the union of the surfaces between the talus and the calcaneus (heel bone). This may require 6-10 weeks of activity restriction, and walking with crutches or using a knee scooter. Once healed, weight-bearing is progressed until the patient is able to walk in regular shoes without the use of crutches. Physical therapy is important to improve ankle motion and balance. Patients can expect a significant improvement in their ability to walk by 3 to 4 months after surgery but, may not reach maximal improvement until 12-18 months after surgery.
Edited July 17, 2017
mf/ 11.6.19