Calcaneal Fracture ORIF: Fractured Heel Bone Surgery
Indications
The term “ORIF” stands for “open reduction, internal fixation.” Quite simply, the surgeon opens the fracture site, puts the fractured heel bone back together then, uses plates and/or screws to stabilize the broken bone pieces. The main indication for heel bone fracture surgery is a displaced calcaneal fracture. Displaced means the bone fragments are “out of position” and may benefit from being “put back together”. A calcaneus fracture (heel bone) commonly includes damage to the subtalar joint. This is the joint that allows side-to-side motion of the foot. A damaged joint can lead to arthritis. By putting these broken pieces back together, the orthopaedic surgeons hope to maximize the functional outcome and reduce the chance that arthritis will develop. However, not all patients with heel bone fractures (calcaneal fractures) are candidates for surgery. Certain heel fractures are not displaced enough to need surgery. For many other patients who have suffered a displaced heel bone fracture the risk of a serious complication (such as a deep infection) may outweigh the potential benefits of surgery.
Surgical Procedure to Fix a Fractured Heel Bone
The goal of surgery to fix a fractured heel bone (calcaneal fracture ORIF) is to place the broken bone fragments back in their original position prior to the injury. By restoring the normal alignment of the heel, the surgeon hopes to provide the patient with the best possible outcome. However, fixing a fractured heel bone can be a challenging endeavor requiring the surgeon to have extensive experience and great skill. It is often the equivalent of trying to put a broken egg back together. The final outcome often depends on the severity of the initial injury. Simple fracture patterns with minimal displacement and large bone pieces are easier to treat than highly complex fractures involving many small pieces. During surgery, these small pieces all need to be carefully placed back in their original position.
During surgery, the patient is usually positioned on his or her side. The incision is made on the outside (lateral) aspect of the foot. The surgeon will determine the type and shape of this incision. Some fractures can be approached through small incisions and others require longer incisions. Once the skin incision is made, the surgeon will carefully move important tendons, nerves, and ligaments out of the way in an effort to visualize the underlying heel (calcaneus) bone and associated fractures. Sometimes these tendons, nerves, and ligaments are damaged along with the calcaneal bone and need to be repaired too. Once the heel bone is exposed, the surgeon will make an effort to inspect the subtalar joint. The subtalar joint, which is often injured in calcaneus fractures, is the joint below your ankle that controls the “side-to-side” (inversion and eversion) motion of your foot.
Once the surgical exposure is complete, the process of systematically reassembling the bone pieces is started. There are usually two primary fragments of the fractured calcaneus. These fragments are realigned first and temporarily fixed with wires to hold them in place. Proper alignment is confirmed by the use of a live x-ray machine (called a C-arm). Next, the subtalar joint surface is reconstructed by systematically repositioning all other fracture fragments. Once the calcaneal alignment is restored, the temporary wires are sequentially removed and replaced with permanent hardware, such as plates and/or screws (Figure 1A and 1B).
The final step involves closure of the surgical wound. In some ways, this is the most important part of the surgical procedure because any breakdown of the wound will increase the risk of a significant post-operative infection. Once the wound closure is complete, a soft cast (called a splint) is applied to the leg.
Figure 1A: Fractured Calcaneus
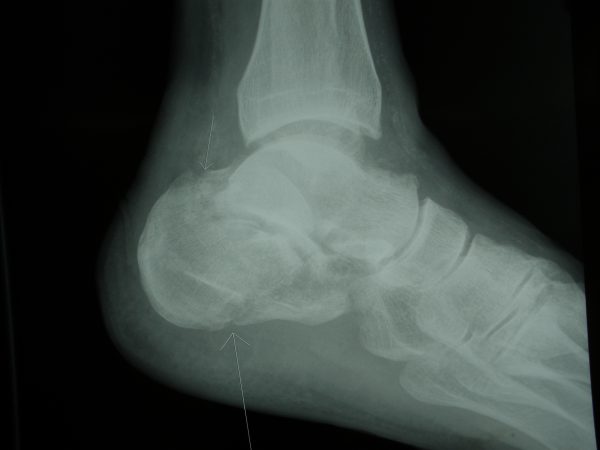
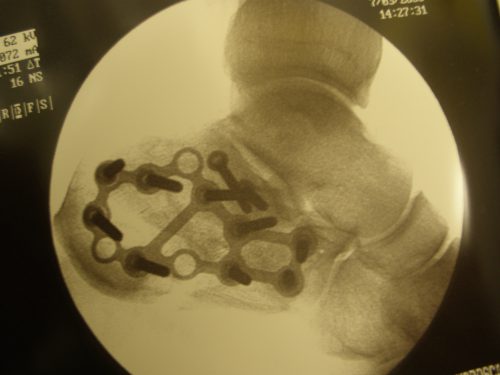
Figure 1B: Fixed Calcaneal Fracture
Recovery from Heel Bone Fracture Surgery
Week 0-2 Post Surgery
The foot is initially immobilized in a well padded cast (splint). Patients should not place any weight on their foot (non weight-bearing). This will require the use of crutches, a walker, a knee walker, and/or a wheelchair. Pain control strategies typically include elevating the foot, using ice to cool the foot, and limiting activities. Pain pills are often initially needed to help manage the post-surgical discomfort. Over-the-counter laxatives and stool softeners may be required to prevent or treat constipation. The dressing should remain clean and dry. The patient should not change the dressing unless instructed by the surgeon.
Week 2-6 Post Surgery
At the first post-operative visit following surgery to fix a fractured heel bone, the surgeon will remove the splint and examine the incision. Sutures may need to be removed. The patient will then be placed either into a cast (which can’t be removed) or a removable boot. For most heel (calcaneus) fractures, the surgeon will ask that the patient remain non weight-bearing until the fracture demonstrates adequate healing – as seen on subsequent x-rays. If you are placed in removable boot, your surgeon may ask that you start a gentle range-of-motion program.
Week 6-12 Post Surgery
During this time period, the patient will be working to improve the range of motion of their foot and ankle. This may involve visits to a physical therapist combined with a home exercise program. The surgeon may also allow a gradually increase in weight-bearing. At the end of this time period, if the fracture shows evidence of solid healing, the surgeon may allow the patient to transition out of the boot and possibly into an ankle brace. The ankle brace will require the use of a wide, stable and comfortable shoe.
Week 12-24 Post Surgery
Once the heel bone has completely healed, the patient will begin more advanced physical therapy activities (such as walking without a limp and continuing with exercises to improve balance and strength). The patient should see a gradual reduction of swelling, although the foot/ankle can remain swollen for many months after surgery. Full recovery from these challenging injuries often takes 12 months or more.
Potential General Complications
- Asymmetric Gait (leading to pain elsewhere)
- Deep Vein Thrombosis
- Failure to Resolve ALL Symptoms
- Pulmonary Embolism (PE)
Potential Specific Complications following Heel Bone Fracture Surgery
- Wound Healing Problems: Although seen with any surgical procedure, wound healing complications are particularly concerning following calcaneal fracture surgery. The area around the outside of the heel has relatively thin skin and limited soft-tissue coverage. This can make wound healing problems more likely following calcaneal fracture surgery, and potentially more severe if they do develop. Wound healing problems are increased significantly for smokers and diabetics.
- Infection: Infections can create a major problem if they occur following a calcaneal fracture. As a result of the limited soft-tissue covering the outside of the heel, a superficial wound infection can quickly spread down to the underlying bone. If an infection develops, the surgeon may recommend the use of oral or intravenous antibiotics. A repeat trip to the operating room may be required.
- Sural Nerve Injury: Injury to the nerve on the outside of the heel (sural nerve) can occur during calcaneal fracture surgery. Nerve injury can occur due to retraction, direct injury, or from scarring during the recovery process. If the sural nerve is injured or cut, the patient may experience numbness or pain along the outside of the foot corresponding to the path of the sural nerve.
- Subtalar Arthritis: Painful subtalar arthritis and stiffness of the hindfoot is common following a heel fracture (calcaneal fractures). This occurs as a result of the damage to the cartilage at the time of the initial injury.
- Painful Hardware: Pain may be associated with the screws and plates used to align and secure the broken bone fragments. This occurs in about 10-20% of patients who have had surgical stabilization of a calcaneus fracture. The surgeon can help you determine if hardware removal is required following heel fracture surgery.
Previously Edited by David Garras, MD, Steven Neufeld, MD, and Matthew Buchanan, MD
Edited June 16th, 2024
sp/6.16.24