Transverse Tarsal Joint Injury-Sprain
(Chopart’s Joint Injury or Midtarsal Injury)
Summary
The transverse tarsal joint, also called the midtarsal or Chopart’s joint, is made up of the joints between the calcaneus and cuboid, and the talus and navicular (Figure 1). It is the joint that connects the hindfoot to the midfoot. A sprain is the most common injury to the transverse tarsal joint and occurs when some or all of the ligaments holding the joint together are torn. The most common mechanism of this injury is an inward twisting and loading of the foot -somewhat similar to the mechanism that causes an ankle sprain. Patients will have significant pain and will often be unable to weight-bear. Diagnosing a transverse tarsal joint injury is made through a combination of patient history, physical examination, and x-ray imaging. Treatment involves rest, anti-inflammatory medications (if tolerated), and immobilization in a cast or walker boot. After the pain and swelling has settled (often a number of weeks) formal physical therapy can be started. Transverse joint sprains typically do not require surgery, although some injuries to Chopart’s joint have associated fractures or dislocation and may require surgery. Although a transverse tarsal joint injury/sprain and an ankle sprain occur via a somewhat similar mechanism with a roughly similar area of injury the length of recovery is usually much longer in patients who have suffered a transverse tarsal joint injury.
Figure 1: Transverse Tarsal Joint (Chopart Joint)
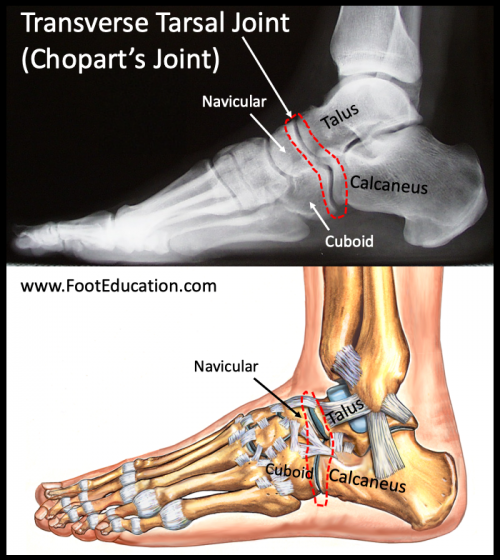
Clinical Presentation
Injuries to the transverse tarsal joint (Chopart joint) occur when the foot and ankle is flexed, twisted (inverted/everted) and loaded at the same time. Therefore athletes, such as football players and gymnasts, are at risk of a Chopart’s joint sprain. Patients will present with immediate pain and swelling on the top (dorsal) and outside (lateral) of the foot. The Chopart’s joint plays a significant role in balance and stability of the foot. Patients will usually not be able to weight-bear after a major transverse tarsal joint injury. Patients may also have bruising over the Chopart’s joint and this bruising can extend to the sole of the foot within a few days of the injury.
Physical Exam
On physical examination patients will be unable to weight bear, or will have significant pain with any attempt to walk. There will be notable swelling around the ankle and midfoot. There will be pain to palpation throughout the injured area. Motion about the ankle and hindfoot will be restricted by pain. In particular, patients will have difficulty twisting the foot inward (inverting) or outward (everting).
Imaging
A Chopart joint sprain may be associated with other ankle injuries. Therefore, while the patient’s history and physical exam may reveal an ankle injury, imaging modalities are useful in establishing the diagnosis, even if this is only to rule out other associated injuries.
X-ray
X-ray of the injured foot will often demonstrate small avulsion fractures of the talar neck or cuboid. These avulsion fractures are indirect evidence that at least part of the ligaments holding the transverse tarsal joint together have been torn. These tiny fractures are stable and occur when the ligament pulls a small area of bone off. This is similar to the way that strong tape stuck to a painted wall may pull off a section of paint if the tape is suddenly ripped off the wall. X-rays can also be used to rule out any major fractures (ex. ankle fracture or Lisfranc injury).
MRI
MRI imaging is not commonly used to aid in the diagnosis of a Chopart’s joint injury. However, it can be helpful if there is concern for a significant injury that would not be seen on plain x-rays. An MRI can reveal evidence of an old transverse tarsal joint injury (Chopart joint sprain) as once this joint has been injured the ligaments will likely remain thickened on MRI imaging -indicative of old injuries.
Treatment of Chopart Joint Injuries
Acute Treatment (first days after injury):
- Rest – Limit weight-bearing to reduce stress on the joint.
- Ice – Apply to decrease swelling and pain.
- Compression – Gentle wrapping can help control swelling.
- Elevation – Keep the foot raised to reduce fluid buildup.
- Anti-inflammatory medication (if not contraindicated) – Helps manage pain and inflammation.
Immobilization Phase:
- Cast or walker boot – Used to keep the foot stable and allow ligaments to heal.
- Crutches – Necessary to avoid loading the injured foot.
- Duration – Usually 3–6 weeks, depending on severity.
- Gentle range of motion – Can be started early, but only within a pain-free range.
Rehabilitation Phase:
- Physical therapy – Key for restoring function, including:
- Muscle strengthening (especially foot and ankle stabilizers).
- Flexibility exercises.
- Gradual return of range of motion.
- Progression – Formal strengthening and higher-level exercises are delayed until pain and swelling have improved.
Surgical Treatment (only in specific cases):
- Considered if there is:
- Marked instability of the Chopart joint.
- Associated injuries such as displaced fractures.
- Surgery may involve fixation of bones or repair of ligaments to restore joint stability.
Edited by Stephen Pinney MD, August 18th 2025