2nd (or 3rd) Metatarsal Stress Fractures
(a.k.a. “March Fractures or Lesser Metatarsal Stress Fractures)
Summary
Lesser metatarsal stress fractures, usually involving the 2nd (or 3rd) metatarsal bone, are associated with pain in the midfoot to forefoot. They typically occur following prolonged or repetitive walking or running and are sometimes called “march fractures.” Risk factors for the development of a lesser metatarsal stress fracture include an increase in activity level, a foot shape that overloads those metatarsals, and/or relatively weak bones (as might be seen with osteoporosis). Some medications that alter the bone composition or low Vitamin D levels may increase the risk of stress fractures. Treatment involves rest and some degree of immobilization usually for between 4 to 8 weeks. It is always useful to identify any underlying problems that contribute to the injury so that this condition can also be treated.
Clinical Presentation
Stress fractures involving the lesser metatarsal bones (typically the 2nd or 3rd) will often present with pain and swelling in the midfoot to forefoot. Frequently, there is an increase in activity, as might be seen when a person goes on a trip that requires increased walking, or when an individual is increasing their training in preparation for a marathon. These injuries are sometimes referred to as “march fractures,” since they can be seen in new military recruits who are going on long hikes. Many people can remember the day or event that their foot pain started. Patients with a large bunion (hallux valgus), often overload the 2nd and 3rd metatarsals predisposing to stress fractures in these bones. Similarly, patients who have a first metatarsal bone that is noticeably shorter than the second metatarsal (known as a “Morton’s Foot) may be at increase risk for a second metatarsal stress fracture. In addition, patients with decreased bone density (osteopenia or osteoporosis), including some young women athletes with irregular menstrual periods (disordered endocrine system), may be at risk as well.
Physical Examination
On examination, there will be some degree of swelling and tenderness directly over the affected metatarsal. There may also be some associated forefoot swelling. Patients usually can walk on the foot, though there will be a limp. Some foot “shapes” are more at risk for stress fractures. Patients with a flatfoot, often with a long second and possibly third toe, are at greater risk of a lesser metatarsal stress fracture. There may also be an associated callus under the ball of the foot, at the base of the second or third toe.
Imaging Study
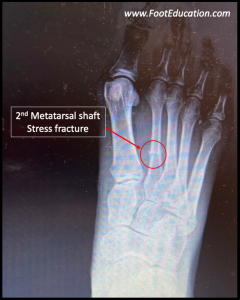
Plain x-rays of the foot may demonstrate subtle signs of a stress fracture. However, in acute stress fractures the actual fracture may not be seen on plain x-rays. Sometimes the fracture may only be seen on plain x-rays two to three weeks after the injury, as it takes this time for enough new bone (callus) to form in response to the stress fracture. A bone scan or MRI will demonstrate a stress fracture or a stress reaction (pre-stress fracture) earlier, and one of these studies may be indicated if the diagnosis is in question.
Metatarsal stress fractures typically occur at the neck region or in the mid-part (shaft) of the bone. Occasionally, high-level ballet and modern dancers will generate stress fractures at the base of the metatarsal, near the midfoot.
Treatment
Non-Surgical Treatment
Most stress fractures can be treated non-surgically. The basic principle is to rest/unload the foot enough to allow more healing than repetitive injury inflicts every day. In some patients, activity modification (break from exercise and minimize walking) may be enough. In others, a surgical shoe or cast boot may help. In a rare few, several weeks of crutches may be required. In general, if the patient is feeling better within 2-3 weeks of diagnosis, they are on the right path. It may take a total of 2-3 months for complete recovery, with occasional patients taking even longer.
Surgical Treatment
Surgery is rarely indicated for a second or third metatarsal stress fracture. Occasionally, there may be an associated non-union that will need to be treated with surgery. Although it is rare, surgery will usually include fixation with a plate and screws, and possibly a bone graft.
Edited on September 13th, 2023
Previously edited by Mark Perry, MD, and Justin Greisberg, MD
sp/9.13.23