Tibialis Anterior Tendonitis – Anterior Tibial Tendonitis
Summary
Tibialis Anterior Tendonitis leads to pain and often swelling in the front of the ankle and into the midfoot. Sometimes the tendon may have degeneration within it as well, and not just inflammation. Symptoms typically occur in middle-aged and older individuals, and are aggravated by standing and walking. Treatment is designed to limit the loading through the tendon and allow the tendon inflammation to settle. Occasionally, tibialis anterior tendonitis will be a precursor to a ruptured anterior tibial tendon. Except in the instance of tendon rupture, surgery is usually not necessary. However, for individuals that have truly failed non-operative management, surgery to clean out the tendon and possibly lengthen the calf muscle may be indicated.
Anterior Tibial Tendonitis Video
Clinical Presentation of Anterior Tibial Tendonitis
Tibialis Anterior Tendonitis is an irritation and swelling of one of the main tendons that lifts the foot up – the anterior tibial tendon which is also known as the tibialis anterior. This condition leads to pain in the front of the ankle or the inside of the midfoot where it inserts on the bone (Figure 1). The condition is often chronic and may also be associated with some swelling in this area. Symptoms tend to occur in patients that are middle-aged or older. Symptoms may be aggravated by increased activity, such as standing and walking.
In a small percentage of patients, anterior tibialis tendonitis will be a precursor to an attritional rupture of the anterior tibial tendon. A rupture of this tendon is usually associated with a sharp pain in the front of the ankle often extending into the inside of the midfoot. Weakness in the ability to bring the foot upward will be noted. Over time, if a rupture of the anterior tibial tendon is missed and not treated there may be increased clawing of the toes, as the tendons to the toes will now be doing most of the work in elevating the foot. Patients may also complain of the foot slapping on the ground when they walk.
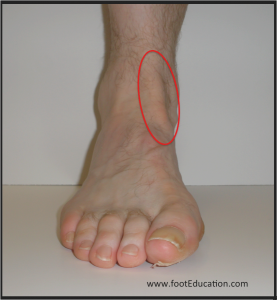
Symptoms of Tibialis Anterior Tendonitis
Examination will often reveal tenderness or even swelling over the anterior tibial tendon in front of the ankle (Figure 2). This is one of the primary tendons that lifts the foot upwards, therefore, resistance to moving the foot upwards (dorsiflexion) will often exacerbate symptoms. There may be a tightness of the calf muscle (equinus contracture).
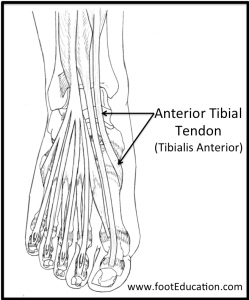
Imaging Studies
Plain x-rays of the foot and ankle are often negative as this is a problem involving a tendon (soft tissue) that will usually not be seen on plain x-rays.
An MRI of this area will reveal swelling and inflammation of the lining of the tendon sheath that the anterior tibial tendon runs through. There will often be fluid around this tendon, and there may be signs of degenerative change within the tendon itself.
Tibialis Anterior Tendonitis Treatment
Treatment of tibialis anterior tendonitis is initially non-operative and is usually successful in settling the symptoms. The treatment involves relative rest of the irritated tendon. This can be done by:
- Limiting activities. This will limit the repetitive load through the tendon. This may be accomplished by limiting standing and walking or any other activities that cause the ankle joint to be repetitively moved. For severe symptoms, it may be beneficial to formally place the patient in a walker boot or cast for a period of a few weeks.
- Anti-inflammatory medications. This can be helpful to settle symptoms if anti-inflammatories can be tolerated.
- Calf Stretching. By stretching the calf, there will be less resistance to elevating (dorsiflexion) the foot. This puts less force through the tendon.
- Ankle-Lacer or (AFO). A brace to stabilize the ankle or to limit the movement through the ankle can help to decrease the load through this tendon, therefore help the symptoms.
- Rehabilitation. Eccentric strengthening programs may be helpful in treating the more chronic symptoms.
Caution: Corticosteroid injections in this region may help settle the symptoms but may increase the risk of rupture of this tendon.
Operative Treatment of Anterior Tibial Tendonitis
In instances where the symptoms of tibialis anterior tendonitis cannot be managed adequately through non-operative management, surgery may be an option. Surgery consists of cleaning out the tendon (debriding) as well as, possibly lengthening out the calf muscle may be beneficial.
Potential Complications
Potential complications include the general complications that may be associated with surgery such as:
- Infection
- Wound healing problems
- Deep Vein Thrombosis (DVT)
- Pulmonary embolism
- Persistence of symptoms
Edited on January 29th, 2024
Previously Edited by Marcus Coe MD, Michael Salamon MD, and Hossein Pakzad MD
sp/1.29.24