Shin Splints (Tibial Periostitis or Medial Tibial Stress Syndrome)
Summary
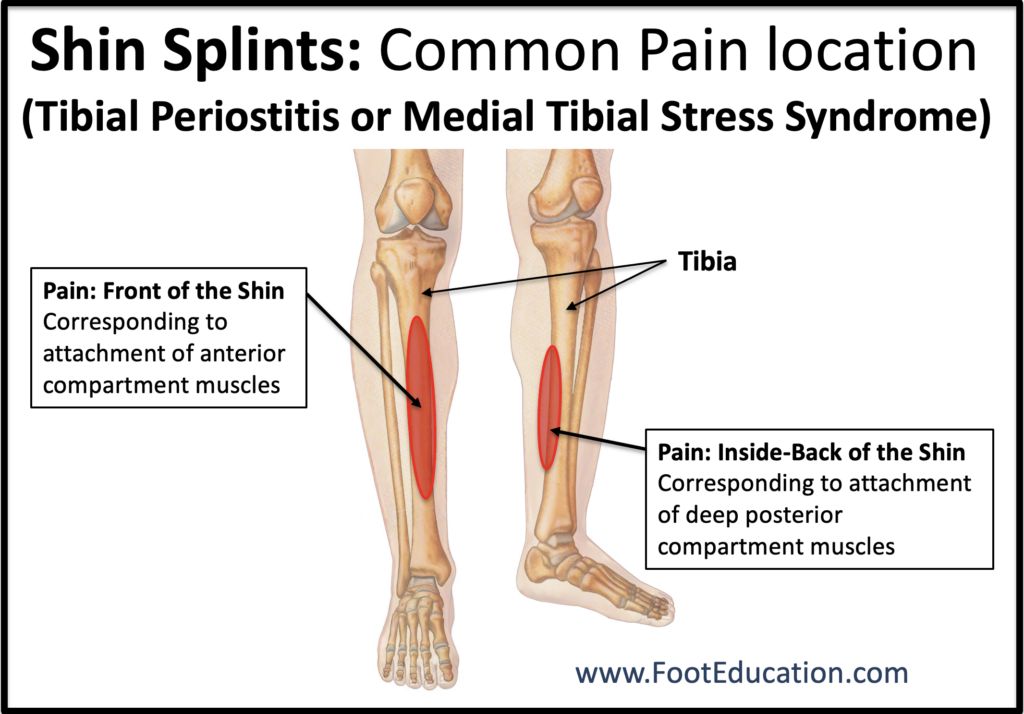
Patients with shin splints experience pain along the front or inner part of their shin (Figure 1). Symptoms are often worse after certain activities or after prolonged rest, such as getting out of bed in the morning. Shin splints commonly develop after a sudden increase in activity level, such as starting a new exercise program, running longer distances, or training on harder surfaces. Treatment usually includes relative rest, icing, anti-inflammatory medications (if appropriate), gentle stretching, and modifying activities until symptoms improve. Shins splints are also known as tibial periostitis or medial tibial stress syndrome.
Clinical Presentation
Pain along the shin bone (tibia) is the most common symptom of shin splints, also known as medial tibial stress syndrome or tibial periostitis. This pain is usually located over a broad area along the front (anterior) or lower inner (medial) part of the shin (Figure 1). Shin splints are often associated with a recent increase in activity, such as increased running, walking on hard surfaces, a new training program, or a long hike. Pain may initially improve once a person warms up and begins exercising. However, with continued activity the pain usually worsens. Start-up pain—pain first thing in the morning or after prolonged sitting—is also common.
Shin splints develop when the tissues that attach muscles to the bone (tibia) become irritated from repetitive stress. The outer layer of the bone, called the periosteum, becomes inflamed due to repeated pulling forces from the muscles attached to it. Several muscles can contribute to this stress. These include muscles in the front of the lower leg (the anterior compartment), such as the tibialis anterior, extensor hallucis longus (which lifts the big toe), and extensor digitorum longus (which lifts the smaller toes). In many cases, the tibialis posterior muscle, which attaches along the inside of the tibia, is also involved and contributes to pain along the inner part of the shin.
Shin splints must be distinguished from a stress fracture of the tibia, which is a small crack in the bone itself caused by repeated stress. Stress fractures usually produce more localized and severe pain than shin splints. However, the symptoms can sometimes overlap, and imaging tests may be required to distinguish between the two conditions.
Shin Splints Physical Examination
During a physical examination, patients with shin splints usually have tenderness along a broad area of the shin bone, particularly along the inner side of the tibia. In some cases there may be mild swelling or redness over the painful area. Many patients also have tight calf muscles, which can increase the pulling forces on the tibia during activity and contribute to the development of shin splints.
Imaging Studies
X-rays of the lower leg bones (the tibia and fibula) may be obtained to rule out a stress fracture. In most patients with shin splints, X-rays appear normal.
In some situations, an MRI scan may be ordered to help distinguish shin splints from a stress fracture. an MRI can show increased fluid or inflammation (called edema) along the outer surface of the tibia where the muscles attach. In contrast, a stress fracture will typically show more localized changes within the bone itself.
Occasionally, a bone scan may be used instead of MRI. During a bone scan, a small amount of radioactive tracer is injected into the bloodstream. Areas of increased bone activity will appear brighter on the scan. In shin splints, the scan usually shows a diffuse, low-level increase in activity along the shin bone, whereas a stress fracture typically shows a more focal and intense area of activity.
Treatment of Shin Splints
Once a diagnosis of shin splints has been made, treatment usually involves two phases: a healing phase, which allows symptoms to settle, and a rehabilitation phase, which helps rebuild strength and reduce the risk of recurrence.
Healing Phase Treatment
Relative Rest
Activities that triggered the symptoms—such as running or jumping—should be reduced or temporarily stopped. Limiting these activities allows the irritated tissues to recover. During this time, lower-impact activities such as swimming or cycling can often be continued to maintain fitness.
Icing
Applying ice to the front of the shin in 10-15 minute intervals can help improve symptoms and decrease the body’s inflammatory response.
Gentle stretching
Stretching the muscles in the front of the lower leg can be helpful. This can be done by gently pointing the foot downward and holding the stretch for 30–60 seconds, repeating it several times a day. Stretching the calf muscles is also beneficial.
Anti-inflammatory medications
A short course of non-steroidal anti-inflammatory medications (NSAIDs) may help reduce pain and inflammation. These medications should not be used simply to mask pain while continuing high-intensity training, as doing so may prolong the injury.
Rehabilitation Phase
Once symptoms have improved, patients can begin a gradual rehabilitation program aimed at safely returning to their previous activity level. Shin splints can recur, so ongoing preventative strategies are often helpful.
Continued stretching
Regular stretching of the calf and lower leg muscles can help reduce stress on the tibia and prevent recurrence.
Heat
Heat applied to the shins may help, particularly in the warm-up phase prior to starting a workout.
Calf support stocking (Shin Splint compression sleeve)
Compression sleeves may provide mild support to the muscles of the lower leg and help reduce muscle vibration during activity. Some athletes find these helpful, although they are not necessary for everyone.
Taping
Some patients benefit from taping techniques designed to reduce stress on the muscles that attach to the shin bone.
Shock absorbing shoes and inserts
Running shoes with good cushioning or shock-absorbing inserts may help decrease the repetitive forces transmitted to the shin during walking or running.
Medial arch supports
Individuals with flat feet or increased foot pronation may benefit from over-the-counter arch supports, which can help improve foot alignment and reduce stress on the tibia.
Graduated return to activity
A gradual return to activity is essential. Training intensity and duration should be increased slowly to reduce the risk of symptoms returning.
Edited by Stephen Pinney MD, March 8th 2026. Previously edited by Steven Neufeld MD .